Initially, the purpose of this blogpost was to entertain the reader (hopefully emergency physician) with the one and only truth about the "mottled skin" since it is a common and frightening sight in the ED but vaguely defined. However, it appears that there is no concrete truth in this case, even major sources (Harrison's online, Merck Manual) are silent as the grave. In the end I found some explanations in on of the two holy bibles in emergency medicine, Rosen's emergency medicine, though in the pediatric section (the other is of course Tintinalli's). I want to belive their description also applies to adults:
Compensated shock can be recognized by the presence of pallor. A pale child with a rapid heart rate should always be considered to be in shock until proved otherwise. As cardiac output is further compromised and perfusion to vital organs is decreased, the skin may become mottled. Mottling is manifested by areas of vasoconstriction and vasodilation in a random pattern on the skin. It reflects loss of small vessel integrity and may be similar to what is seen in vital organs during multiple organ system failure. Mottling is usually an ominous sign. It is important to not confuse cutis marmorata with mottling in young infants [...]. Cutis marmorata is a lacy marbling of the skin caused by vascular instability. It is a normal finding and is commonly seen in infants in a cool ambient environment.
Cutis marmorata
 is sometimes mentioned along with shock but there are other more common differential diagnoses such as decompression sickness, normal (cold) response in young children and a congenital variant (CMTC). All indicate instability in the vasculature (vasospasm/dilation). The patterns are unfortunately not uniformly defined as seen in the pictures on DermAtlas and NEJM.
is sometimes mentioned along with shock but there are other more common differential diagnoses such as decompression sickness, normal (cold) response in young children and a congenital variant (CMTC). All indicate instability in the vasculature (vasospasm/dilation). The patterns are unfortunately not uniformly defined as seen in the pictures on DermAtlas and NEJM.
Livedo reticularis
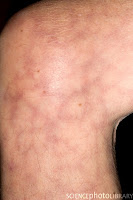 is also connected with shock, as in this case in BMJs "Images in emergency medicine" series. It confuses however my view of the phenomenon whereas other sources describe livedo as a common pattern of various well-defined, mostly autoimmune, diseases ranging from benign to acute ischemia of the extremities. The skin pattern is sharper than cutis marmorata and the morphology more reticular, as the name indicates.
is also connected with shock, as in this case in BMJs "Images in emergency medicine" series. It confuses however my view of the phenomenon whereas other sources describe livedo as a common pattern of various well-defined, mostly autoimmune, diseases ranging from benign to acute ischemia of the extremities. The skin pattern is sharper than cutis marmorata and the morphology more reticular, as the name indicates.So after all the browsing I unfortunately didn't come to any intelligent conclusions; for "mottled skin" in the shocked patient, there is no good definition or specific description and differentiation from other similar symptoms pictures of more benign origin. What is clear (as before!) however is that this is a pattern that all emergency physicians must be aware of as it commonly indicates a disaster on its way.

No comments:
Post a Comment